lifestyle
Microdosing GLP-1 Agonists: 9 Things Doctors Won't Tell You

Ana Reisdorf, MS, RD - GLP-1 expert
Feb 18, 2026

You've probably heard whispers about microdosing GLP-1 in online forums, from friends who've lost weight, or even from your doctor's office. The idea sounds appealing: taking smaller doses of these powerful medications to manage weight, blood sugar, and metabolic health while potentially dodging harsh side effects. But here's the problem: the internet is flooded with conflicting advice, anecdotal success stories, and questionable claims that leave you wondering what's actually safe and effective versus what's just wellness trend noise.
That's where tools like MeAgain's GLP-1 app become essential. Instead of piecing together fragments of information from random sources, you get access to evidence-based guidance that helps you understand dosing strategies, track your response to treatment, and make decisions grounded in science rather than social media hype. The app cuts through the confusion, providing personalized insights aligned with your health goals while keeping safety front and center.
Summary
Microdosing GLP-1 medications has attracted over 10,000 participants in physician-supervised programs, but the term describes wildly different practices depending on who's using it. Some patients work with doctors to adjust FDA-approved doses, while others purchase unregulated compounded versions or stretch prescribed supplies to reduce costs. The FDA has explicitly linked compounded GLP-1 medications to hospitalizations, creating a critical distinction between medical dose adjustment and self-directed experimentation with untested formulations.
Clinical trials established GLP-1 dosing protocols through years of safety and efficacy testing, but no published research supports microdosing strategies circulating on social media. Research by physicians such as Dr. Mitch Biermann at Scripps Clinic examines maintenance dosing after patients achieve results on standard protocols, which differs fundamentally from starting treatment with non-standard doses. Between 10 and 20 percent of female patients in specialized practices achieve significant results on the lowest standard dose of tirzepatide (2.5mg weekly), but most eventually require 5 to 7.5mg during active weight-loss phases.
Cost barriers drive much of the microdosing interest, with patients facing roughly $500 monthly out-of-pocket expenses for medications that insurance won't cover for weight loss. When patients ration medication by stretching supplies or taking reduced doses to save money, they're making decisions based on financial constraints rather than medical response. This creates contamination risks, dosing inconsistencies, and side effect patterns that cycle repeatedly because medication never reaches steady therapeutic levels in the bloodstream.
The biological paradox of reduced dosing catches many patients off guard. Taking inconsistent or inadequate amounts means the medication clears between injections, causing each dose to trigger initial side effects like nausea and gastrointestinal distress without allowing the body to adapt. Patients end up experiencing maximum discomfort with minimal therapeutic benefit, creating worse outcomes than consistent standard dosing that allows the body to reach a steady state and adjust over time.
Studies show that patients who discontinue GLP-1 medications typically regain lost weight as hunger hormones intensify and metabolic rate decreases in response to weight loss. The body defends its set point through hormonal regulation that operates outside conscious control, making temporary medication use followed by willpower-based maintenance biologically implausible for most people. This reality means effective treatment requires viewing GLP-1 medications as long-term management tools rather than temporary interventions while building habits.
GLP-1 app addresses this by consolidating injection timing, dose tracking, side effects, protein intake, hydration, and weight changes into structured documentation, transforming physician conversations from vague descriptions into pattern-based decisions when adjusting protocols.
Table of Contents
9 Things Doctors Won't Tell You About Microdosing GLP-1 Agonists
Make Your GLP-1 Microdosing Journey Easier with MeAgain—Try MeAgain
Should You Microdose GLP-1 Drugs?
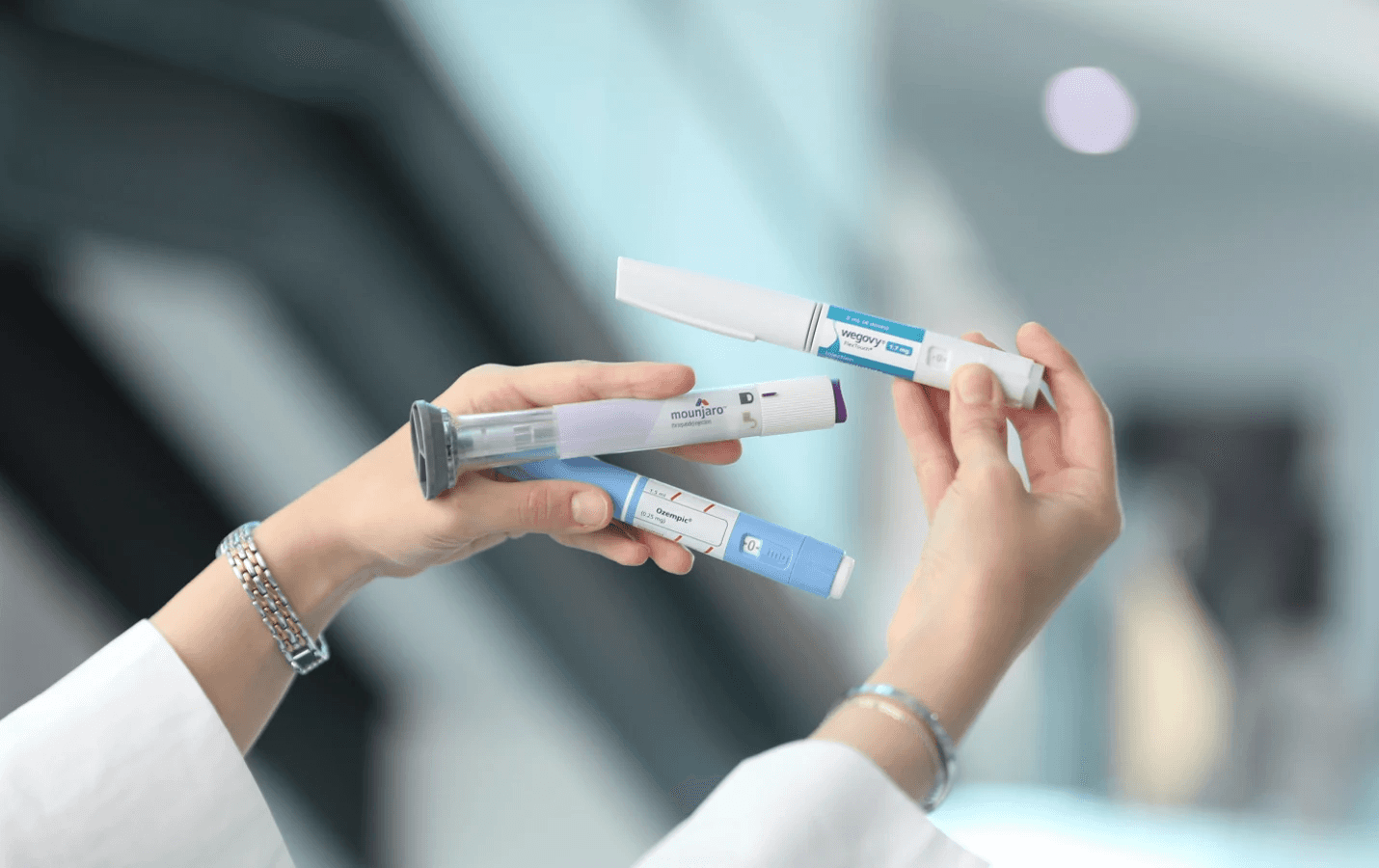
The conversation around microdosing GLP-1 medications has grown loud enough that it's hard to ignore. Patients who struggle with standard doses, people frustrated by cost barriers, and those who've heard celebrity endorsements are all asking the same question: Is this a legitimate path forward, or just another wellness trend dressed up as medical innovation? The answer depends on what you mean by "microdosing" and whether you're working with a physician or experimenting on your own.
The term itself creates confusion before you even start. "Microdosing" isn't regulated, which means it describes wildly different practices depending on who's talking. For some, it means purchasing compounded versions of semaglutide or tirzepatide from international manufacturers or specialty pharmacies to access non-standard doses. For others, it means remaining on the lowest FDA-approved dose rather than gradually increasing it as clinical trials recommend. For a third group, it means using a syringe to draw up smaller portions of their prescribed medication, stretching a month's supply over six weeks to save money.
These aren't the same thing. Not even close. When Dr. Jeffrey Egler, Noom's chief medical officer, noted that more than 10,000 people have signed up for programs exploring lower-dose GLP-1 strategies, he was describing physician-supervised protocols, not self-directed experimentation. The distinction matters because one approach involves medical oversight, regular monitoring, and adjustments based on your body's response. The other involves guesswork, a risk of contamination, and no safety net if something goes wrong.
What Drives People Toward Microdosing?
Cost sits at the center of this conversation. Most insurance companies don't cover GLP-1 medications for weight loss, leaving patients to pay out of pocket. Even with recent price reductions through direct-to-consumer programs, you're still looking at around $500 per month. When you're facing that bill indefinitely, the math becomes painfully simple: if you can make one vial last six weeks instead of four, you've just cut your annual spending by thousands of dollars.
Side effects create the second major pressure point. Nausea, vomiting, diarrhea, and severe constipation make standard dosing intolerable for some patients. The hope is that a lower dose delivers therapeutic benefits without the gastrointestinal misery. It's a reasonable desire, but the biology doesn't always cooperate. When you take a reduced dose, the medication clears your system faster than intended. The next time you inject, your body treats it like a first dose again, triggering the same side effects you were trying to avoid. You end up cycling through discomfort without ever achieving the steady medication levels that allow your body to adapt.
Access issues compound the problem. Drug shortages that began after the 2021 and 2022 FDA approvals left patients scrambling for alternatives. Availability still varies by region and pharmacy. When you can't get your prescribed medication reliably, the temptation to ration what you have becomes overwhelming. Studies document that patients who stop GLP-1 medications typically regain the weight they lost, creating pressure to stay on treatment no matter what it takes.
The Critical Distinction Between Dose Adjustment and Microdosing
Physicians adjust medication doses constantly. It's standard medical practice across every therapeutic area. If you're experiencing side effects from a GLP-1 medication, your doctor might slow the escalation schedule, keep you at a lower maintenance dose, or switch you to a different formulation. This is not microdosing. This is medicine. Microdosing compounded versions, by contrast, means using medications that haven't been FDA-verified for safety, effectiveness, or quality. Compounding pharmacies create these versions using similar ingredients to FDA-approved drugs, but without the regulatory oversight that ensures consistency batch to batch. The FDA has explicitly linked compounded GLP-1 medications to hospitalizations. When you're drawing up portions of medication yourself using a syringe and vial, you face real contamination risk and the possibility of accidental overdosing.
Dr. W. Scott Butsch, an obesity medicine subspecialist, draws a hard line here: "I don't recommend using compounded versions of these medications because they're untested, both in their effectiveness and their safety." The distinction isn't about being overly cautious. It's about recognizing that we have robust clinical trial data showing how to start these medications safely, but zero data supporting alternative approaches.
What the Evidence Actually Shows
Anecdotally, people report losing weight on microdoses of GLP-1 medications. Bravo TV host Andy Cohen told the TODAY show that microdosing helped him lose "a good chunk of weight." The Washington Post published stories about patients experiencing fewer side effects with lower doses. These accounts are real, but they don't constitute evidence that the practice is safe or effective. Dr. Nidhi Kansal, an internal medicine specialist at Northwestern Medical Group, clearly highlights the gap: there is no published research supporting the recommendation to microdose a GLP-1 drug. Clinical trials tested specific dosing protocols. Those protocols established both safety and efficacy. When you deviate from them, you're conducting an experiment with a sample size of one and no control group.
The situation becomes more complex for patients who achieve their health goals on lower doses. If you started on 2.5mg of tirzepatide, increased to 5mg, and saw your weight stabilize along with improvements in metabolic markers, what's the right maintenance dose? Should you continue escalating to the FDA-approved maximum of 15mg, or can you stay at 5mg indefinitely?
Dr. Mitch Biermann, an internal medicine and obesity medicine specialist at Scripps Clinic, is researching this exact question. His unpublished study data suggest that spacing medication dosing might be a maintenance strategy. Some patients in his study take their medication every 10 days instead of weekly. Others stretch it to every two weeks. A handful go even longer while maintaining their weight. But here's the critical point: these patients didn't start with non-standard doses. They followed FDA protocols, reached therapeutic levels, achieved their health goals, and then worked with physicians to find maintenance strategies. That's the opposite of starting with microdoses and hoping for the best.
The Protocol Gap Nobody Talks About
Dr. Biermann's observation cuts to the heart of the confusion: "We have tons of trials that tell us how to start these medications. We have none that tell us how to stop them." The asymmetry creates a genuine dilemma. Patients who respond well to lower doses want guidance about long-term management. Physicians want evidence-based protocols for weaning or maintenance dosing. Neither exists yet.
The FDA regulates brand-name GLP-1 drugs in very specific doses, as Dr. Katy Williams, a bariatric medicine specialist at MU Health Care, explains. Those doses emerged from clinical trials designed to establish safety and efficacy. When you step outside those parameters, you're in uncharted territory. That doesn't automatically make it dangerous, but it does mean you're making decisions without the safety net of clinical evidence. The American Diabetes Association doesn't endorse microdosing. No official medical guidelines support it. The federal government's recent initiative to lower GLP-1 drug costs represents progress toward making evidence-based treatments more accessible, but it doesn't resolve the underlying tension between what patients can afford and what protocols recommend.
When you're experimenting with dosing strategies, tracking becomes essential, not optional. You need to monitor how your body responds to different doses, document side effects, watch for patterns in your hunger signals and energy levels, and record weight changes over time. Without systematic tracking, you're flying blind. Tools like MeAgain's GLP-1 app provide a structured way to track injection timing, protein intake, hydration, side effects, and progress in one place. When you're working with your physician to find your optimal dose, that data becomes the foundation for informed decisions rather than guesswork.
What Actually Deserves Serious Consideration
If you're struggling with standard GLP-1 dosing, the answer isn't to start experimenting on your own. The answer is to have an honest conversation with a physician who understands these medications. Dose adjustments occur frequently in medical practice. Staying at the largest dose you can tolerate rather than escalating to the maximum is a legitimate clinical decision, not a failure. If cost is the barrier, explore direct-to-consumer programs that offer significantly lower prices. If side effects are intolerable, ask about slower escalation schedules or alternative formulations. If you've achieved your health goals on a lower dose, discuss maintenance strategies with your doctor. These are medical decisions that benefit from medical expertise.
What doesn't deserve serious consideration is purchasing compounded versions from unregulated sources, drawing up your own doses without medical supervision, or following protocols based on celebrity anecdotes rather than clinical evidence. The risks aren't theoretical. Contamination, overdosing, and inadequate therapeutic levels create real harm. The weight loss and metabolic improvements from GLP-1 medications are remarkable. Patients describe feeling like themselves again after years of struggling. But those outcomes depend on using these medications as they were designed and tested. When financial barriers or side effects make that impossible, the solution is better access and better medical support, not unsupervised experimentation.
Your journey with GLP-1 medications is deeply personal. The dose that works for you might look different from what works for someone else. But personalization doesn't mean improvisation. It means working with knowledgeable physicians, tracking your response systematically, and making adjustments based on evidence rather than hope. The question isn't whether microdosing can produce weight loss. The question is whether it does so safely, sustainably, and with enough medical oversight to catch problems before they become serious. For most people asking about microdosing, what they need is a physician willing to thoughtfully adjust their protocol and a system for carefully tracking their response. But before you can make that decision, you need to separate fact from fiction about what microdosing actually involves and what the risks really are.
Related Reading
Thinking About Microdosing GLP-1? 5 Myths Debunked
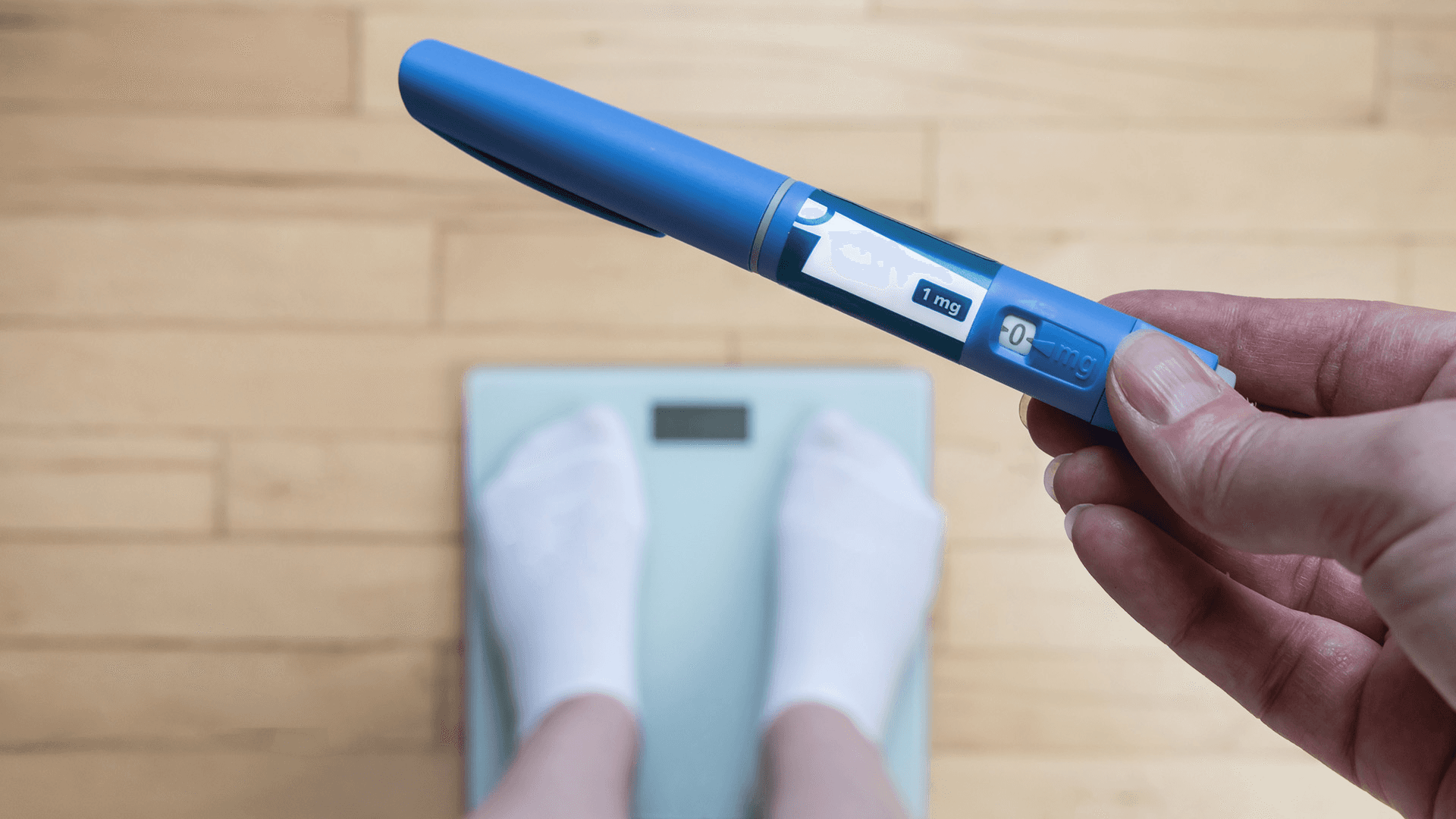
Microdosing GLP-1 medications sits at the intersection of medical innovation and social media hype, making it nearly impossible to distinguish legitimate medical practice from dangerous experimentation. The medical establishment warns against unregulated compounded medications while online communities share transformation stories that sound too good to ignore. What you need is clarity about what's actually true, what's dangerously false, and what falls somewhere in between. Five myths dominate the conversation. Each one contains just enough truth to sound plausible, which makes them particularly dangerous.
1. Myth One: Microdoses Are Just Smaller Versions of FDA-Approved Medications
The FDA-approved GLP-1 medications come in prefilled, single-dose pens. Each pen contains exactly the amount prescribed for one injection. You can't split them into smaller doses without creating contamination risk and measurement inconsistency. To create what people call "microdoses," pharmacies compound the medication from scratch, mixing ingredients to create custom formulations.
Compounded medications bypass the FDA approval process entirely. The FDA regulates brand-name GLP-1 drugs in very specific doses, as Dr. Katy Williams explains. Those doses emerged from years of clinical trials testing safety and efficacy. Compounded versions might contain the same active ingredient, but you have no guarantee about purity, concentration, or sterility. Best case, you're getting exactly what you paid for. Worst case, you're injecting something that varies batch to batch with no quality control protecting you.
The distinction matters because when patients experience side effects or lack of efficacy, there's no way to know whether the problem stems from the dose, the formulation, or contaminated ingredients. You're experimenting without the safety net that makes medical treatment predictable.
2. Myth Two: You Can Use Microdosing Temporarily While Building Healthy Habits
This myth feels intuitively correct. Take a low dose of medication to quiet food noise and cravings while you establish exercise routines and healthier eating patterns. Once those habits stick, taper off the medication and maintain your weight through willpower and discipline.
The biology doesn't cooperate. Your hypothalamus regulates body weight through hormonal signaling that operates completely outside conscious control. When you lose weight, your brain interprets it as starvation and responds by increasing hunger hormones, intensifying food cravings, and reducing metabolic rate. These aren't psychological responses you can overcome with better habits. They're physiological adaptations designed to restore your body to its previous weight.
The moment you stop taking GLP-1 medication, regardless of dose, those hormonal signals return at full strength. The habits you built while medicated are subject to biological pressures that willpower can't match. Dr. Williams sees this pattern repeatedly: patients lose ten pounds on low doses, stop the medication, feel confident, then gradually regain the weight as their hunger signals overwhelm their new routines. If you want to maintain weight loss, you're looking at lifelong medication, not a temporary tool.
3. Myth Three: Microdosing Works Great If You Only Need to Lose a Little Weight
The appeal here targets people who sit just above their ideal weight, maybe fifteen or twenty pounds they'd like to lose without the commitment or side effects of full-dose GLP-1 treatment. It sounds reasonable. Why use a sledgehammer when you need a chisel?
The problem is that all medications carry risk. FDA-approved GLP-1 medications at standard doses have been studied extensively. We know the risk-benefit profile for people with moderate to severe obesity. Research shows that losing 15% to 20% of body weight produces measurable improvements in cardiovascular health, diabetes risk, and metabolic function. For someone carrying significant excess weight, those benefits clearly outweigh the risks.
If you're trying to lose 5% or less of your body weight, the math changes. The health benefits become marginal while the risks remain constant. Lifestyle modifications deliver that level of weight loss without medication risk. Dr. Williams is direct: work on your lifestyle first. Your physician can identify specific changes that will produce five to ten pounds of weight loss without exposing you to medication side effects or requiring lifelong treatment.
4. Myth Four: Microdosing Delivers the Same Health Benefits as Standard Dosing
This myth extends beyond weight loss to the broader metabolic benefits researchers have discovered. GLP-1 medications improve insulin sensitivity, reduce cardiovascular disease risk, and show promise for conditions like Type 1 diabetes and polycystic ovary syndrome. If you can get those benefits at lower doses with fewer side effects, why wouldn't you? The catch is that only FDA-approved doses have been studied for these additional benefits. The clinical trials that documented cardiovascular improvements, gains in insulin sensitivity, and improvements in metabolic health markers all used standard dosing protocols. Whether those same benefits appear at substantially lower doses remains unknown. No published research supports it.
Dr. Williams acknowledges the medications show remarkable promise, but emphasizes that we simply don't know whether low doses produce the same effects. If you're considering microdosing primarily for metabolic benefits rather than weight loss, you're making a decision without evidence. Lifestyle interventions deliver proven metabolic improvements without the uncertainty.
When you're navigating dose adjustments, whether working with your physician on a supervised protocol or managing side effects, tracking is the difference between informed decisions and guesswork. You need to document how different doses affect your hunger, energy levels, side effects, and weight changes over time. Most people try to track this mentally or across multiple apps, which makes pattern recognition nearly impossible. Tools like MeAgain's GLP-1 app consolidate injection timing, protein intake, hydration, side effects, and progress into a single view. When you're working with your physician to find your optimal dose, that comprehensive data transforms conversations from vague descriptions to specific patterns.
5. Myth Five: Getting a Prescription Online Is Just as Good as Seeing Your Doctor
Telehealth has dramatically expanded access to GLP-1 medications. You can get a prescription from a licensed physician without leaving your house. For people in rural areas or without nearby specialists, this represents genuine progress. The myth is that all prescriptions are equivalent regardless of who writes them. The physician prescribing your medication through an online platform doesn't know your health history. They don't have access to your other medications, your lab results, or the context that makes your situation unique. GLP-1 medications interact with blood thinners, hormonal birth control, and other common drugs. Without comprehensive knowledge of your health, those interactions get missed.
More fundamentally, GLP-1 medications are most effective when used as part of comprehensive lifestyle changes, not as a standalone treatment. Before prescribing these medications, physicians should discuss what you're committing to over the long term, review the risks and benefits specific to your situation, and establish monitoring protocols. Dr. Williams emphasizes that not everyone is a suitable candidate for GLP-1 treatment. Making that determination requires the kind of relationship and knowledge that fifteen-minute video consultations can't provide. The online physician might be excellent and well-intentioned. But they're working with incomplete information and have no ongoing relationship to monitor your response over time. When you're taking a medication indefinitely, that continuity of care matters more than convenience.
These five myths share a common thread. They all make microdosing sound simpler, safer, and more straightforward than it actually is. The reality involves more nuance, greater uncertainty, and a greater need for medical oversight than social media suggests. Clearing away these misconceptions doesn't answer whether microdosing makes sense for you. It just removes the false certainty that makes bad decisions feel safe. What physicians know but rarely discuss openly is where the real insight lives, and those unspoken realities change everything about how you should think about this decision.
Related Reading
Can You Take Semaglutide Every Other Week For Weight Loss
How Old Do You Have To Be To Take Ozempic
How To Ask Your Doctor For Weight Loss Injections
9 Things Doctors Won't Tell You About Microdosing GLP-1 Agonists
Microdosing GLP-1 medications exists in a strange medical gray zone where conflicting information from established institutions and online communities makes it nearly impossible to separate legitimate medical insight from dangerous speculation. What physicians know from clinical experience but rarely articulate publicly shapes how you should think about dosing strategies, side-effect management, and long-term sustainability. These aren't secrets kept deliberately. They're nuanced observations that don't fit neatly into official guidelines or fifteen-minute appointments.
1. Some Patients Respond Powerfully to Doses Below Clinical Trial Thresholds
Clinical trials establish therapeutic ranges based on population averages. Semaglutide studies tested weekly doses of 0.25mg, 0.5mg, 1mg, and 2.4mg. Tirzepatide trials evaluated doses of 2.5mg, 5mg, 7.5mg, 10mg, 12.5mg, and 15mg. Those became the FDA-approved doses because they produced statistically significant weight loss across large patient populations.
Individual biology doesn't care about population statistics. Dr. Varun Andres Sasson, founder of Lighthouse Weight Loss, a telemedicine practice specializing in GLP-based treatment, observes substantial variability in patient responses. "There is a lot of variability in how patients respond to GLPs. You won't know how strongly or how weakly they affect you until you try them." In his practice, 10 to 20 percent of female patients achieve significant results on 2.5mg of tirzepatide weekly, the lowest standard dose, never requiring escalation during active weight loss phases.
This creates a genuine dilemma for physicians. Official guidelines recommend dose escalation until patients reach therapeutic levels proven in clinical trials. But when a patient loses weight steadily, experiences appetite suppression, and shows improved metabolic markers on a lower dose, what's the medical justification for increasing? You're adding side effect risk and medication cost without a clear benefit for that specific person. The catch is you can't predict who will respond to lower doses before starting treatment. Body weight, metabolic health, insulin sensitivity, and genetic factors all influence GLP-1 receptor sensitivity. Two people with identical BMI and health histories can require dramatically different doses to achieve the same outcomes.
2. Microdosing Research Exists, But It's Not What You Think
When physicians say "there's no research on microdosing," they mean no published clinical trials have tested the specific protocols circulating on social media. That's accurate but incomplete. Dr. Mitch Biermann at Scripps Clinic is actively researching maintenance dosing strategies that involve spacing injections beyond the standard weekly interval. His unpublished data suggests some patients maintain weight loss by taking medication every 10 to 14 days instead of weekly.
This represents a fundamentally different approach than starting with non-standard doses. Patients in Dr. Biermann's study followed FDA protocols, achieved their health goals at approved doses, and then worked with physicians to identify minimum effective maintenance levels. The research question isn't whether you can lose weight starting with tiny doses. It's whether you can maintain the results achieved with standard dosing by reducing the frequency or amount afterward.
Dr. Varun Andres Sasson, who lost more than 40 pounds himself on standard GLP-1 doses, articulates a treatment philosophy many physicians share privately but hesitate to state publicly. "My personal treatment philosophy is that patients should take the lowest possible dose that gets them to their weight loss or health goals. They should then try weaning down the dose to see if they can maintain results at lower doses, possibly even microdoses." The distinction matters enormously. Starting low and hoping for results differs completely from achieving results first, then carefully reducing under medical supervision. One approach has emerging research support. The other remains purely speculative.
3. Off-Label Prescribing Happens Constantly, Including for GLP-1 Medications
Dr. Jennifer Warren, who specializes in obesity management and founded Physicians' Healthy Weight Center, addresses the reality physicians navigate daily. "Physicians have always been allowed to prescribe off-label. In certain scenarios, using drugs like metformin or antidepressants off-label is literally the standard of care. In those cases, if the doctor didn't prescribe off-label, they're not practicing good medicine." When a patient experiences uncontrollable vomiting or severe diarrhea on the lowest FDA-approved dose, physicians face a choice. Discontinue the medication entirely, accepting that the patient loses access to potentially life-changing treatment. Or prescribe a lower dose, perhaps one-tenth of the starting dose, to see whether the patient can tolerate it while still experiencing some benefit.
Dr. Warren explains the practical reality: "If someone had uncontrollable vomiting or diarrhea, a doctor might prescribe a lower dose. It's called off-label prescribing. And it works for many patients. They can often still lose noticeable amounts of weight, but it may happen more slowly." This isn't reckless experimentation. It's physicians using clinical judgment to balance potential benefits against known risks for specific patients. The difference between this and unsupervised microdosing is medical oversight, documentation of response, and adjustment based on objective outcomes rather than social media testimonials.
Dr. Pippert, whose full name and credentials weren't provided in the source material but whose clinical observations appear throughout medical discussions of GLP-1 dosing, notes that as physicians gain experience with any medication, they naturally adjust approaches based on what they observe. "As providers, when we begin to use a medication, it is natural to observe how the medication works and adjust our approach and dosing regimen based on our experience and observation." Official guidelines provide starting points, not absolute rules. The challenge is distinguishing between thoughtful clinical adjustment and random experimentation.
4. The Side Effect Paradox Nobody Warns You About
Lower doses should theoretically produce fewer side effects. The logic seems bulletproof: less medication means less gastrointestinal disruption, less nausea, less vomiting. Dr. Pippert confirms this holds true for some patients. "In my experience I have seen patients benefit from this strategy." But biology creates a paradox. GLP-1 medications work by maintaining steady blood levels that your body gradually adapts to. When you take inconsistent doses or amounts too small to maintain therapeutic levels, the medication clears your system between injections. Each new dose reaches your body as if it were the first exposure, triggering the same initial side effects repeatedly.
You end up experiencing nausea, fatigue, and gastrointestinal distress cyclically without ever reaching the steady state where your body adjusts, and side effects diminish. It's worse than taking a consistent therapeutic dose because you never escape the adaptation phase. Dr. Pippert emphasizes this risk directly. "It is easy to lose sight of the fact that these are powerful medications, which is why they are so effective, that can cause side effects and complications even at low dose. With minimal to no oversight or instruction, there is a meaningful risk of problems."
The paradox extends to effectiveness. Patients microdosing to avoid side effects sometimes discover they're experiencing all the discomfort with minimal therapeutic benefit. They've created the worst possible outcome: maximum suffering, minimum results.
5. Most Patients Eventually Need Higher Doses Than They Initially Hoped
Dr. Sasson's clinical experience reveals a pattern patients rarely anticipate. While 10 to 20 percent of his female patients respond powerfully to the lowest standard dose, "most women in my practice end up on 5 to 7.5mg weekly during the active weight loss phase" of tirzepatide treatment. This creates a psychological challenge. Patients start treatment hoping they'll be the exception who responds to tiny doses. They read social media posts from people who lost substantial weight on microdoses and assume their experience will mirror theirs. When it doesn't, they face a choice: increase the dose and accept they need more medication than they hoped, or persist with inadequate dosing while their results stall.
The biology behind this is straightforward. Your body defends its set point weight through hormonal regulation. The more weight you lose, the stronger the compensatory signals become. Hunger hormones increase. Metabolic rate decreases. Food becomes more rewarding neurologically. GLP-1 medications counteract these signals, but only at doses sufficient to override your body's defensive response. If you start with doses too low to produce meaningful GLP-1 receptor activation, you're fighting your body's set point defense with insufficient ammunition. Some people win that fight through sheer metabolic luck. Most don't.
Tracking becomes essential when you're trying to find your minimum effective dose. You need objective data demonstrating whether a given dose produces appetite suppression, weight loss, and metabolic improvements, or whether you're merely hoping for results with no change. Most people rely on memory and general impressions, which makes pattern recognition impossible. Platforms like MeAgain's GLP-1 app provide a structured way to document injection timing, dose amounts, hunger levels, side effects, protein intake, and weight changes in a single consolidated view. When you're working with your physician to determine whether your current dose is working or whether you need an adjustment, that documented pattern becomes the foundation for informed decisions rather than guesswork.
6. The "Microdosing Movement" Includes Practices With Wildly Different Risk Profiles
When Dr. Tyna Moore, a naturopathic physician licensed in Oregon, describes her microdosing approach, she's referring to something fundamentally different from what most patients mean by the term. Moore teaches a $2,300 course for clinicians on GLP-1 protocols and shares her strategies with more than 86,000 YouTube subscribers. Her approach involves doses "so low, I could barely see it in the syringe," cycled on and off to "keep cellular receptors listening." Moore describes remarkable results from this protocol: "Just absolute clearance of brain fog, mood improvement, joint pain decrease, skin improvement, all kinds of wonderful." These outcomes extend beyond weight loss into broader wellness claims that haven't been tested in clinical trials.
The challenge is distinguishing between Moore's medically supervised protocols, developed through her clinical practice and training, versus patients drawing up arbitrary amounts from compounded vials purchased online. Both get labeled "microdosing," but the risk profiles differ enormously. Moore works with patients under her medical license, monitors their response, and adjusts protocols based on outcomes. A patient buying compounded semaglutide from an international supplier and injecting untested amounts based on YouTube videos faces contamination risk, dosing errors, and zero medical oversight if complications arise. Dr. Pippert warns explicitly about this distinction. "To be clear, microdosing of GLP-1 medications is not included in any official guidelines. With minimal to no oversight or instruction, there is a meaningful risk of problems."
7. The Longevity and Anti-Aging Claims Outpace the Evidence
A 2024 paper posted on a preprint server found that semaglutide slowed several biological markers of aging in people with an HIV-related condition, causing abnormal fat accumulation. The paper generated substantial attention in longevity communities and among GLP-1 influencers. It's currently undergoing peer review. Varun Dwaraka, director of research at TruDiagnostic and one of the paper's authors, addresses the gap between preliminary findings and clinical recommendations directly. "Is semaglutide ready to be used for antiaging? I don't necessarily think that we're just there yet." That cautious assessment gets lost when the findings circulate through social media. Patients see headlines about GLP-1 medications slowing aging and assume the science is settled. They start microdosing not for weight loss but for longevity benefits that remain hypothetical.
The biological plausibility exists. GLP-1 medications reduce inflammation, improve insulin sensitivity, and decrease cardiovascular disease risk. All of these factors correlate with healthier aging. But correlation isn't causation, and biological markers aren't equivalent to actual improvements in lifespan or healthspan. Michaela Robbins, a nurse practitioner who founded East x West Med, a telehealth practice focused on hormone care and longevity, articulates the frustration many practitioners feel. "We take too long. With traditional medicine, we have long, rigorous trials at the expense of individuals that could potentially see a benefit from it when we have an understanding of what potential risks are."
The tension is real. Waiting for definitive clinical trials means people who might benefit don't get access for years or decades. But acting before evidence exists means exposing patients to unknown risks for unproven benefits. Aging isn't recognized as a treatable condition by the FDA, which makes it challenging to design and fund formal clinical trials. Without that research infrastructure, the longevity claims around GLP-1 microdosing will likely remain in this gray zone for years.
8. Cost-Driven Microdosing Creates Different Risks Than Medically-Supervised Low Dosing
Christine Babb's story illustrates the economic pressure driving microdosing adoption. She purchased compounded tirzepatide through a telehealth firm after hearing about GLP-1 medications from coworkers who lost weight. She paid approximately $800 for a supply she expects will last until February, substantially longer than the standard four-week supply period. Babb hasn't consulted with a doctor about adjusting her dose. "I don't want to live forever," she said. "I just want to live well." The sentiment is understandable, but it reveals how cost barriers push patients toward self-directed experimentation.
When you're stretching a month's supply across six weeks to reduce costs, you're not following a deliberate protocol designed to find your minimum effective dose. You're rationing medication because you can't afford the prescribed amount. The distinction matters because your dosing decisions are driven by financial constraints rather than medical response.
Dr. Jennifer Warren acknowledges the economic reality shaping these decisions. "It's probably not harmful when done with guidance from your physician. It just may not work as well as getting full therapeutic doses. Those were the doses deemed most effective in clinical trials for GLP-1 agonists." The "probably not harmful" qualifier is critical. We have extensive safety data for FDA-approved doses taken at prescribed intervals. We have essentially no data on compounded versions taken at arbitrary amounts across inconsistent schedules. The absence of widespread reported harm doesn't prove safety. It might just mean we haven't been tracking the right outcomes or watching long enough.
9. Traditional Medicine Moves Too Slowly for Patients Facing Immediate Decisions
The fundamental tension underlying the entire microdosing conversation is timing. Rigorous clinical trials take years to design, fund, execute, and publish. Peer review adds months. Replication studies extend the timeline further. By the time medical consensus forms around optimal dosing strategies, individual patients have already made decisions based on incomplete information. Michaela Robbins captures this frustration from a practitioner's perspective. "We take too long," she says of traditional medical research. The patients in her practice can't wait five years for definitive answers about maintenance dosing or longevity benefits. They need treatment decisions now.
But speed creates its own risks. Dr. Varun Andres Sasson, despite his optimistic view of GLP-1 potential, states clearly: "Microdosing is interesting but untested. We just don't know how well it works because it hasn't been studied." That uncertainty doesn't stop patients from trying. It just means they're experimenting without the safety infrastructure that makes medical treatment predictable. When you take an FDA-approved medication at the prescribed dose and experience a serious side effect, reporting systems capture that data. Future patients benefit from your experience through updated warnings and revised protocols.
When you take a compounded version at a non-standard dose and experience problems, that information disappears into the void. No reporting system captures it. No database tracks it. The next patient, considering the same approach, has no access to your experience. We're conducting thousands of individual experiments with sample sizes of one and no mechanism for learning from the results collectively.
The Real Question Isn't Whether Microdosing Works, But Whether It Works for You
Dr. Pippert's clinical experience reveals the core truth physicians understand but struggle to communicate in sound bites. "In my experience I have seen patients benefit from this strategy." Some people respond powerfully to doses below standard therapeutic levels. Others need maximum doses to achieve modest results. Most fall somewhere in between. The variability means there's no universal answer to whether microdosing makes sense. Dr. Sasson emphasizes this directly: "You won't know how strongly or how weakly they affect you until you try them." Your response depends on factors that can't be predicted from BMI, age, or metabolic health markers alone.
This creates an impossible situation for patients seeking clear guidance. The honest medical answer is "try it under supervision and track your response carefully." That's not the definitive recommendation people want, but it's the only one supported by current evidence. Dr. Sasson offers a framework that makes sense in light of the uncertainty. "My personal treatment philosophy is that patients should take the lowest possible dose that gets them to their weight loss or health goals." Start with proven protocols. Achieve your objectives using doses we know work. Then carefully experiment with reduction to identify your minimum effective maintenance level.
That approach inverts the microdosing logic circulating on social media. Instead of starting low and hoping for results, you start with proven effectiveness and work backward toward the minimum dose that sustains your outcomes. The difference is that you're reducing from a position of success rather than building on speculation. Dr. Sasson adds context from his personal experience losing more than 40 pounds on standard doses of GLP-1. "GLPs are so remarkable for overall health that I think microdosing is worth considering." But that consideration should happen after you've experienced the full therapeutic benefit, not as a substitute for proven treatment. But knowing what doctors think privately is only half the picture, because what you do with that information determines everything.
Make Your GLP-1 Microdosing Journey Easier with MeAgain—Try MeAgain
Whether you're working with your physician to find your optimal dose or following standard protocols, the medication represents only one variable in a much larger equation. Muscle preservation, protein targets, hydration consistency, and fiber intake determine whether your weight-loss journey delivers the body composition and energy levels you want. Most people focus entirely on the injection while ignoring the daily habits that compound into results or sabotage them entirely.
MeAgain's GLP-1 app transforms those daily disciplines into an engaging experience with a capybara companion that turns protein goals, water intake, and movement into something that feels less like obligation and more like progress you can see. When you're experimenting with dosing strategies, systematic tracking becomes mandatory. You need documented patterns showing how your body responds to different approaches, what side effects emerge at various doses, and which combination of medication and lifestyle produces the outcomes you're after.
The Journey Card feature captures every milestone, creating a visual record of your experimentation that becomes essential when you're changing this fast and need to understand what's actually working versus what just feels like it might be. Download MeAgain today and build the support system your microdosing journey deserves, because the medication gets you started, but the daily work determines where you end up.
Related Reading
Best Place To Get Wegovy Online
Best Place To Buy Tirzepatide Online
503a Pharmacy Tirzepatide
Best Place To Get Mounjaro
Top Semaglutide Providers
Cost Of Oral Wegovy
Best Place To Get Semaglutide
Microdosing Glp 1
Tirzepatide Compound Cost
